|
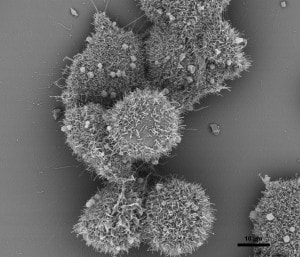
The nature of The Beast - Colon cancer cells. Cancer survivors have an understanding of each other. We belong to an exclusive club. It’s not a club that you strive to join. “You have cancer” are the three words that gain admittance to the club - and surviving, of course. We don’t do high-fives when we hook up with each other at our local cancer clinic for appointments. Those are usually somber affairs. But social media has allowed us to communicate with each other. We join online support groups that allow us to talk to one another about our experiences, about chemo, and about our oncs. We have our own language - onc(s), scanxiety, NED among other words. Many of us have our own name for our cancer. I call mine The Beast. We don’t distinguish between races because cancer is a disease that knows no racial or class boundaries. One of the things we celebrate is when our CT scan is NED. NED means No Evidence of Disease. More specifically it means that our cancer is in complete remission. It doesn’t mean we’re “cured” of cancer. It means that cancer hasn’t been detected by the scan. Yet, there are nagging doubts about NED and complete remission. Go to any cancer support group and you’ll hear those doubts expressed. It is probably one of the most talked about topics among survivors. It’s not that we don’t have faith in our doctors. We’ve lived in the bright sunshine of survivorship until a dark cloud of recurrence blots it all out. And recurrence happens to too many of us. As a Stage IV survivor, I’m inquisitive about this disease that I have. I spend a lot of time reading books and articles about The Beast. I do so because I want to know my enemy. Recently I read “The Death of Cancer” by Vincent T. DeVita Jr., M.D., and Elizabeth DeVita-Raeburn. It’s not the type of book that most survivors would read. Unless, like me, they are inquisitive. It’s not bogged down with indecipherable scientific/medical terms. It’s a well written memoir, understandable, and a page-turner. One early passage made me sit up: “But we have to be smart about what we hit them with – and how aggressively. Cancer cells are uncannily adaptive; they learn to outwit therapies quickly. So the first attempt to treat a cancer has the best odds of curing it, because we’re hitting it with something it’s never seen before. The cancer is more treatable than it will ever be again. This is one reason why recurrences are so troubling: you’re dealing with much smarter cells by then.” The last sentence was particularly troubling to me because of my own recurrence in 2016. My recurrence was a surprise to me and my onc. But I’m jumping ahead in my narrative. I have to go back to the beginning to where this all started before I can get to the two and a half billionth cell. My sojourn in Cancerland began April 16, 2013. As a result of anemia and black, tarry stools, my doctor at the Native American Community clinic, Katie Bickel (ANP), referred me to Dr. Melton-Meaux, a colon and rectal specialist at U of M Physicians. A colonoscopy was performed on April 26. The pathology results of the colonoscopy were “Malignant partially obstructing tumor cecum.” Alarmed by the results of the colonoscopy, Dr. Melton-Meaux ordered a CT scan which was performed on May 1. The results of the scan were a “lobulated mass involving the distal cecum and ascending colon consistent with known colon carcinoma…There are multiple lymph nodes in the medial mesentery to ascending colon. The size and number are worrisome for possible metastic involvement.” Because of the size of the tumor and its location, Dr. Melton-Meaux decided that surgery should be done as quickly as possible. On May 14, she performed laparoscopic surgery and removed my ascending colon and associated lymph nodes. The surgical pathology report from May 16 states that the tumor was Adenocarcinoma, i.e., the type of tumor in my colon. Adeno means glands and carcinoma is the type of cancer. Adenocarcinoma develops in the lining of the colon (or rectum). The size of my tumor was 9.5 x 5.5 x 3.0 cm and the gross measurement 2.5 cm. It was considered to be a very large tumor, hence Dr. Melton-Meaux's urgency in performing surgery. There was a bowel wall invasion with the tumor infiltrating into it, but not through the muscularis propria. The muscularis propria is a deep, thick layer of muscle that contracts to force along the contents of the intestines. The lymph nodes were all negative, meaning the cancer hadn’t invaded them. Under AJCC Cancer Staging, my cancer was listed as T2, N0, M0, G2. More specifically, T2 means that cancer has grown into the muscularis propria; N0 means no cancer in nearby lymph nodes; M0 means that cancer has not spread to other parts of the body, i.e., no metastasis; and G2 means the cells are somewhat like healthy cells and are called moderately differentiated. Cancer is divided into four stages - I, II, II, IV. Mine was classified as Stage I: The cancer had grown through the mucosa and had invaded the muscular layer of the colon. It had not spread into nearby tissue or lymph nodes Following my surgery I was assigned to an oncologist, Dr. Edward Greeno, to handle my case. In his first oncologist report, Dr. Greeno wrote: Stage 1 colon cancer. The patient has had a complete resection. His risk of recurrence is quite low. His risk is low enough that he need not worry about adjuvant chemotherapy. We should have some minimal followup to watch for evidence of recurrence. I recommended a CEA level and physical exam every 3 months until we are 2 years out, and then every 6 months until we are 5 years out. According the American Cancer Society, the 5-year relative survival rate for people with stage I colon cancer is about 92%. What this means is that an estimated 92 out of 100 people who have colon cancer are still alive 5 years after being diagnosed. However, many of these people live much longer than 5 years after diagnosis. Things were looking pretty good. I was in a group with a high survival rate and chemo wasn’t required. My surgeon, Dr. Melton-Meaux, tacked on yearly colonoscopies as part of my 5-year surveillance program. This was because in a post-surgery colonoscopy on May 28, 2014, multiple hyperplastic (non-pre-cancerous) polyps were removed. Overall, my cancer team was taking good care of me. I didn’t take my annual colonoscopy on schedule in 2015. I waited until January 2016. Three polyps were removed - two were hyperplastic and one was an adenoma polyp. Adenoma polyps are pre-cancerous. They can take seven to ten years to develop into cancer. An adenoma polyp was how it all started for me. Prior to my surgery in 2013, an adenoma polyp had evolved into a tumor. It had been incubating in my colon for seven to ten years. Had I gotten a colonoscopy in my fifties as recommended, I wouldn’t be writing any of this. Almost three years later, cancer was once again trying to reestablish itself in my colon in the same manner that it did previously. It wasn’t cancer per se. It wasn’t recurrence. But the conditions were ripe for it to become cancer in several years. Of course, this was worrisome to me. I thought I was done with The Beast. But here it was again trying to make a reappearance. In May 23, 2016, I had my annual CT scan. It was the third scan of my 5-year surveillance program. I expected it to be like my previous scans - uneventful and NED. I had the scan early in the morning and met with Dr. Greeno in the early afternoon for the results. After greeting me, the first thing Dr. Greeno said was: “Well, Robert, we found something on your scan.” Both my wife and I were crestfallen. We knew this wasn't going to be good news. What was found was a secondary malignant neoplasm of the liver. My colon cancer had metastasized as a lesion on the left lobe of my liver. Dr. Greeno ordered a PET scan for the next day to see if the cancer had metastasized elsewhere, e.g., the lymph nodes. It hadn’t. As a result of my recurrence, my status as a cancer survivor changed to Stage IVA, meaning the cancer has spread to another organ. The 5-year survival rate for Stage IV is 13%. Although the outlook is poor, the cancer can be held in check, i.e., remission, with treatment if the cancer is limited to a small area. In my case, the recurrence was limited to the left lobe of my liver. When I asked Dr. Greeno how the cancer had reached my liver, he said the cells had to have passed through my bloodstream. The occurrence of such is extremely low with Stage I, but it does happen. With my recurrence, the two and a half billionth cell had found its mark. In his book, Dr. DeVita writes: It is unrealistic to use survival as an end point. Consider the number of cancer cells a drug has to kill to be effective. The average patient with advanced cancer has more than a kilogram of tumor on board. That’s many billions of cancer cells, because a lump about one centimeter across contains roughly one billion cells. Even after surgery, when a primary cancer has been removed and no errant cells can be detected, a patient can have more than a billion cancer cells circulating around the body. Consider that the original gross measurement of my colon tumor was 2.5 cm. This would mean that there were roughly two and a half billion cancer cells in my tumor. Granted, the tumor was removed and, along with it, billions of cancer cells. However, as DeVita notes, more than a billion cells continue to circulate in the body. My use of the term “two and a half billionth cell” is simply a point of reference. The main point is that errant cancer cells circulated in my bloodstream and made their way to the left lobe of my liver and established a beachhead. The treatment for my recurrence included four rounds of neoadjuvant chemo - Oxaliplatin infusion with daily doses of Capecitabine tabs. Originally, six rounds of infusion were scheduled; however after a severe reaction to round four, the neoadjuvant chemo was cancelled. In November, 2016, the left lobe of my liver was removed via open surgery. I was in OR for nine hours. Three hours for the liver surgery and six hours to remove an incisional hernia that had developed after my colon surgery in 2013. My liver surgeon, Dr. Eric Jensen, said I was clean - no other cancer was found in my body. I then went through twelve rounds of adjuvant chemo - Irinotecan, which is used for metastatic colon cancer. I was put on a high-surveillance program – CT scans every three months for two years followed with CT scans every six months for three years. My scan this month (October) will complete the two years of my surveillance program and then I will go to the three year program. Of course, I’m comforted by my doctors keeping a watchful eye on me. Yet, there is the nagging thought that I am just another two and a half billionth cell away from metastases. But in writing this, it isn’t my intention to be a cancer doomsayer. There is always uncertainly living with cancer. Yet, today there are targeted treatments and immunotherapy that can provide a survivor with a good, quality life. There may never be an overall cure for cancer, but today’s advancements allow us to manage it and live with it. Complete remission may be the talk of the town in cancer support groups. But that's because we know the reality of complete remission. The two and a half billionth cell is still there. In some cases, it will find us, in other cases it will be held in check with treatment. For survivors, we know that somewhere deep The Beast lurks. Approach it with a respectful fear. But live life as the Creator intended. © 2018, Robert DesJarlait
0 Comments
|
Robert Desjarlait
|

 RSS Feed
RSS Feed
